You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Pediatric Sedation for Dental Treatment: Safety and Compliance
John R. Ayre, DDS
Pediatric sedation is a valuable adjunct to treatment in many cases where behavior management is necessary. Sedation can be defined as a drug-induced depression of consciousness. Proper safety and training can ensure successful sedation; however, due to the unpredictable nature of children, it is imperative to approach each situation carefully. According to the American Academy of Pediatrics (AAP), the responsibility of pediatrics begins with the fetus and continues through 21 years.1 This article focuses primarily on minimal to moderate sedation.
Successful Pediatric Sedation
Minimal to moderate sedation refers to a drug-induced state during which patients can respond verbally to commands. Cognitive function and coordination may be impaired, but ventilatory and cardiovascular functions remain unaffected. The latter are the most challenging aspects of this technique.2 Preparation is necessary to manage the reality that some children are more prone to slipping into deeper sedation, which could result in impairment of cardiovascular and ventilatory function. It is important to remember that children cannot be treated as small adults when it comes to sedation.3 A 2006 study concluded that safety is often dependent on how well a sedation system can manage less-serious events.4
Sedation is considered a means for increasing the likelihood of successfully providing dental care. However, parents may believe that sedation can compromise their child's health. For this reason, a series of guidelines have been created for the monitoring and management of pediatric patients during and after sedation. The guidelines were prepared jointly by the AAP and the American Academy of Pediatric Dentistry (AAPD).5
Responsible practitioners, based on their judgment, may exceed the level of monitoring and care outlined in the guidelines, but they should never do less than the guidelines recommend. Also, although the guidelines are intended to encourage high-quality patient care, adherence to them cannot guarantee a specific patient outcome. In dentistry, the demand for anesthesiology services is growing.6 Pediatric dentistry programs are expected to follow AAPD guidelines.7
One of the main purposes of sedation is to control behavior. Specific factors will have an impact, including the child's level of cooperation, past history of bad experiences, the extent of the work to be completed, and the needs presented by the parents, who may be concerned about insurance or may have a time-sensitive situation. These elements can affect a treatment's sedation goals. Clinicians must guard the patient's safety and welfare while minimizing discomfort and controlling behavior.
Safety and Risk Factors in Sedation
There is a risk that some children will fall rapidly into deep sedation and stop breathing. Fatalities have occurred.2 Deep sedation is not generally achievable with nitrous oxide alone and requires an additional sedative agent.8Children are more vulnerable during sedation because of their youth, anatomy, and other factors. A study examining the results of 50,000 sedation and anesthesia procedures held at 37 locations found that children younger than 6 years have a greater risk of adverse events.9 No deaths were recorded in this study, but airway obstruction occurred approximately 2,800 times. The authors concluded that sedation safety depends on a practitioner's ability to manage the less-serious events.
Anatomically, children younger than 6 years have a small airway that can be easily blocked. The size difference between a 4-year-old and a 12-year-old is significant. Additionally, enlarged tonsils can dramatically increase the chance of airway obstruction. Also, very young children do not have as high an oxygen reserve in their blood as older children or adults, whose bodies are more capable of compensating for short lapses. Overweight and obese children merit special consideration because sedation drugs are stored in fat cells. A sedative will not be metabolized as quickly, which creates a longer recovery time.2,10
Drug Considerations
A 2016 study on nitrous oxide used as a sedative found a low occurrence of adverse effects but noted that vomiting was the most prevalent issue, dependent on the use of concomitant opioids.11 Nitrous oxide use has grown over time, but so has public concern over its safety.12 One of the most commonly used oral sedation agents is midazolam, which is considered desirable because it is safe, works quickly, and results in just a small amount of amnesia.13,14 Midazolam spray through a buccal route has also been studied for use on children who demonstrate poor intranasal administration compliance.15 In some cases, drug combinations such as meperidine and hydroxyzine are used for oral sedation.16 A study from 2009 concluded that children with developmental disabilities have a threefold higher risk of life-threatening complications during sedation.17 That conclusion is an example of why it is not always appropriate for sedation to be used as a first-line treatment for cavities. There are lower-risk and less-invasive options, such as placing a temporary filling using silver diamine fluoride or delaying treatment.
A careful preprocedural review of the patient's underlying medical considerations or condition may minimize, but not completely eliminate, adverse responses, including hypoventilation, apnea, airway obstruction, laryngospasm, and cardiopulmonary impairment. Clinicians must carefully consider how the sedative process could impact a patient based on the patient's unique medical history.18 Drug selections should be made based on the intended purpose.19 Moreover, there should always be staff members present with the skills necessary to rescue patients from an adverse response.
The AAP and AAPD have both stated emphatically that at-home pre-sedation "poses an unacceptable risk."5 Practitioners should thus not prescribe any medications before the patient comes to the office. It is also advisable to remind well-wishing parents not to administer anything on their own. Occasionally parents feel they are being helpful by giving medication to their child before the appointment. This is doubly problematic because the practitioner will not know the amount administered or how it may interact with anything given during the appointment.
Safe sedation of children requires a systematic approach, including the primary guideline: medical supervision.20 Monitoring of a sedated child must be accomplished by focusing on the depths of sedation.21 Practitioners are responsible for the safety of the child.22 If there is any medical concern, a medical consultation is necessary. A pre-sedation evaluation is critical as well. Fasting is another important point: parents should be directed that their child not have foods or liquids after midnight before the treatment. They must be vigilant not to leave snacks or drinks within arms' reach. To prevent confusion, saying "nothing after midnight" is preferable to explaining a specific number of hours for fasting.
Airway Management
To perform an examination of a child's airway, the clinician may choose one of two methods: the Mallampati score, which evaluates the size of the airway, or the Brodsky scale, which evaluates tonsil size. Whichever method is chosen, the clinician must ensure that the back of the throat can be observed to determine whether the tonsils are obstructive or whether there may be any other concerns. Clinicians must also have thorough knowledge of the medications to be administered, including mechanisms of action and awareness of conditions under which the medication can be dangerous. Any drugs for which there is no reversal agent should be avoided.5
Airway management training is crucial.23 Cardiopulmonary resuscitation (CPR) courses are also essential, as well as familiarity with skills such as a simple chin thrust or placing a laryngeal mask airway (LMA) (which must be easily located in the office). Rescue equipment on hand should be a priority, but it must be age-appropriate. Clinicians should have the appropriate reversal agents at the correct dosage for the specific sedation depending on whether they are using a narcotic or benzodiazepine. Trained auxiliary personnel are also key. For example, the practice must have a dedicated assistant whose sole job is to monitor vital signs.
Other Precautions
In some locations, a certain number of dental personnel must be present during the sedation. A dental assistant who monitors the patient must be CPR-certified and have proper monitoring equipment, including a blood pressure cuff, pulse oximeter, and precordial stethoscope. There should be a well-staffed recovery area for the patient after the procedure, whether it is the initial operatory or a separate room. Finally, discharge criteria must be met and the child returned to near pre-sedation levels. The child should be able to talk and walk out. One possibility is to have the child stop at a "prize box" on the way out of the office as a good distraction that also demonstrates to the clinician the alertness level of the child. One of the office staff or an assistant should follow the parent and child to their car to make sure the child is put appropriately into the vehicle.5
Handling the Sedation Record
A sedation record is a medical form and legal document that must be filled out legibly with blue or black ink. Any mistakes should be crossed out and initialed, and the record should not have any doodles or drawings on it. A copy of the AAPD sedation record form can be found on the association's website.24 Clinicians should use this form to better understand the patient's health history, but they must also assume that parents may be likely to omit or incorrectly fill out some information on the assessment. This could be a result of assuming that other medical situations are not applicable to a dental procedure. The clinician may need to ask detailed questions regarding history of premature birth, any past experiences with respiratory syncytial virus (RSV) or asthma, the last time the child was hospitalized, snoring, and more. The form must be very legible, to the point where it could be read clearly as a legal document enlarged in a courtroom. The document must communicate that a compelling reason exists before making the decision to use pharmacologic therapy.
Successful sedation begins with the patient selection area of the form. Patient selection is the primary means by which sedation safety is secured.25 The clinician should use this section as a guide to choose whether conscious sedation or intravenous (IV)/general anesthesia will be most effective. Factors such as the child's age, temperament, cooperative nature, medical conditions, caries risk status, desire to complete the work in one visit, urgency of treatment, and the amount and type of work required are all documented in this area. Also documented are classification, any need for medical consultation, and the treatment plan.
Clinicians should incorporate a protocol of "no relation, no sedation." A signature of a parent or legal guardian must be obtained. A grandparent who is not a legal guardian or an individual with a permission slip from the parent will not suffice. Furthermore, clinicians must follow the guideline of informed consent, which compels the dentist to discuss risks, benefits, and alternatives to any therapy. Health literacy and language barriers can impact a parent's ability to understand written documents. According to a recent US Department of Health and Human Services study, 14% of American adults (approximately 30 million people) fall below the basic level of health literacy.26 This fact underscores the importance of drafting a carefully worded, easy-to-understand consent form and discussing it adequately with the child's parent or legal caregiver before administering any sedation.
It is helpful to use a practice protocol where a signed informed consent copy is given to the parent along with paperwork that provides some clarifying information or background on the treatment. One way to check whether parents have read the preoperative sedation paperwork is to include a line about midway through the preoperative instructions that asks, for example, the name of the clinician's favorite family movie. On the day of the appointment, the ability of the parent to answer this question may influence the clinician's willingness to proceed with sedation. The parent must have read the instructions and must understand what to expect of the sedation.
The sedation record will also include an assessment for the day of the sedation. This is the most important section, because by the time it is completed, the clinician will have a good indication of the likelihood of sedation success. It is also the clinician's last chance to prepare the parent for possible outcomes and explain expectations. The clinician should again emphasize that oral conscious sedation is not general anesthesia27,28 and the goal is not to put the child to sleep. Clinicians should also remind parents that not all sedations are successful because every patient reacts differently. It must be made clear to the parent that if the child reacts poorly to sedation, the clinician will terminate treatment and reschedule for a time when IV29 or general anesthesia can be administered. It is much easier to provide clarification and warnings before the start of treatment rather than excuses after the fact.
Drug dosage calculations are another portion of the form. The dosages and maximum dose must be noted. It is particularly necessary to know this information if the clinician is administering any opioids or narcotics because they can cause respiratory depression. Also, clinicians absolutely must understand emergency reversals. The clinician should be as detailed and clear as possible when recording intraoperative management, postoperative monitoring information, and discharge, paying close attention to the discharge vital signs area of the form. The clinician can complete the form while having parents schedule a follow-up visit for 2 or 3 weeks later. The blood pressure cuff should be used again, bringing the child up to at least a halfway-seated position to get assessment numbers.5
After the procedure, the discharge process should be discussed carefully with the parent or guardian; each box on the discharge form should be fully reviewed and checked off. Specific points should be reviewed with parents/guardians, and they should be given a clear means to contact the dentist on a more direct line, such as a cell phone. They should then sign the bottom, signifying the child is being turned over to them. They should be asked for their after-hours number because it may be different from what is in the chart.
It should be reiterated to the parents/guardians that the child should not be left alone or unattended. Siblings and babysitters of all ages should not be considered responsible guardians. A 2014 study found that in a sample of 50 children, 66% slept in the car and 12% were difficult to awaken.30 The final section of the form is the dentist and two assistants who participate in the sedation. Lastly is a line to note the postoperative call. Parents/guardians will likely appreciate the time the clinician takes to call them. They can even put the child on the phone and have the child say how he or she is doing.
Emergency Supplies and Equipment
State boards and legislative rules largely determine the equipment that must be purchased for an office to sustain a distressed patient. The office must take time to regularly review equipment: for example, determining whether the portable oxygen tank is full and whether all medications are stocked completely. The clinician should be familiar with the state's most recent set of requirements.
Some practices may find it beneficial to invest in a sedation room that encourages calm and relaxation. In this room, all preoperative vital signs can be taken and medications can be administered. The patient and parents/guardians can be given a blanket, and the light can be turned off. An assistant can check on the parents/guardians and child while they watch television or otherwise relax.
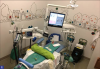
For the operatory setup (Figure 1), a papoose board may not be used for treatment, but it can function as a means of flattening the chair. Velcro straps should only be employed if the child becomes uncooperative and the clinician just needs to finish temporizing. Parental consent must be obtained before employing the use of a papoose board or other form of protective stabilization. Otherwise, it is best not to wrap the child during treatment. The exception is a special needs child.31 In a 2016 review of parent perceptions of sedation, 75% of parents surveyed felt protective stabilization was unnecessary and 87% wanted to stay with their children.32A traditional operatory setup will include an extra tank of oxygen, a crash cart, a place for assistants to sit while they monitor heart rate and blood pressure, a precordial stethoscope, blankets, instructions for reversal medications, a self-inflating bag, and an emergency kit (Figure 2). For the emergency kit, it is important to know when it was last opened and whether all employees are familiar with the contents.5
The office should have an emergency medical plan, and all the employees should be familiar with its protocol (Figure 3). It should be based on the number of team members in the office. The actions of the team in an emergency should be detailed, and the team should be prepared to follow them. The protocol should be reviewed regularly, especially if there is personnel turnover. It is helpful to know who will orchestrate the flow of the rest of the practice and how others in the practice can be notified. An individual should have a dedicated responsibility of bringing in emergency personnel. This person should stand in front of the building and direct emergency medical services (EMS) personnel.33
State Compliance
Rules and regulations can vary widely from state to state. However, it is incumbent on the clinician to know those rules and contact the state dental board to be educated on them, while also ensuring the practice is compliant. An excellent resource is the Pediatric Anesthesia Study conducted by the Dental Board of California.34 The information and conclusions reported have become the basis for many state laws and regulations related to the sedation of children. It is also good to recognize that some states have passed specific regulations regarding sedation, such as Hawaii, where Finley's Law dictates that any dental office using general anesthesia or deep-to-moderate sedation is required to post a sign with the state's consumer protection agency contact information. In many states, on-site inspections are now mandatory.33,35
Overall, state legislators are taking a serious look at how children are being sedated. Dentists must behave and practice in a manner that will protect the dental field's right to sedate patients. If an emergency occurs, the front-office person should document every step for legal purposes. This documentation should include the names of all team members who participated; the time, date, and location of the sedation; medications administered before, during, and after the procedure; vital signs recorded; the time EMS was called; the time EMS arrived; communication to the EMS team; and follow-up with child and parents/guardians.
Conclusion
Sedation is a valuable tool for the dental treatment of children and special needs patients. However, because lower-risk and less-invasive treatment options are available, sedation should not be considered the first-line treatment for all cavities. A lower-risk and less-invasive option should be discussed with parents before proceeding to treatment that may be more serious. Clinicians must note that pediatric patients require careful consideration before undertaking any sedation procedures, with risks evaluated thoroughly and all guidelines followed. Safety and preparation of the entire dental team are essential for a successful treatment.
About the Author
John R. Ayre, DDS
My Kid's Dentist and Orthodontics
Conroe, Texas
References
1. American Academy of Pediatrics, Council on Child and Adolescent Health. Age limit of pediatrics. Pediatrics.1988;81(5):736.
2. Nelson, TM, Xu Z. Pediatric dental sedation: challenges and opportunities. Clin Cosmet Investig Dent. 2015;7:97-106.
3. Attri JP, Sharan R, Makkar V, et al. Conscious sedation: emerging trends in pediatric dentistry. Anesth Essays Res. 2017;11(2):277-281.
4. Cravero JP, Blike GT, Beach M, et al. Incidence and nature of adverse events during pediatric sedation/anesthesia for procedures outside the operating room: report from the Pediatric Sedation Research Consortium. Pediatrics.2006;118(3):1087-1096.
5. Coté CJ, Wilson S; American Academy of Pediatrics; American Academy of Pediatric Dentistry. Guidelines for monitoring and management of pediatric patients before, during, and after sedation for diagnostic and therapeutic procedure: update 2016. Pediatr Dent.2016;38(4):e13-e39.
6. Hicks CG, Jones JE, Saxen M, et al. Demand in pediatric dentistry for sedation and general anesthesia by dentist anesthesiologists: a survey of directors of dentist anesthesiologist and pediatric dentistry residencies. Anesth Prog.2012;59(1):3-11.
7.Morin A, Ocanto R, Drukteinis L, Hardigan PC. Survey of current clinical and curriculum practices of postgraduate pediatric dentistry programs in nonintravenous conscious sedation in the United States. Pediatr Dent.2016;38(5):398-405.
8. Kim SO, Kim YJ, Hyun HK, et al. Deep sedation with sevoflurane inhalation via a nasal hood for brief dental procedures in pediatric patients. Pediatr Emerg Care. 2013;29(8):926-928.
9.Cravero JP, Beach ML, Blike GT, et al. The incidence and nature of adverse events during pediatric sedation/anesthesia with propofol for procedures outside the operating room: a report from the Pediatric Sedation Research Consortium. Anesth Analg. 2009;108(3):795-804.
10. Kang J, Vann WF Jr, Lee JY, Anderson JA. The safety of sedation for overweight/obese children in the dental setting. Pediatr Dent. 2012;34(5):392-396.
11. Tsze DS, Mallory MD, Cravero JP. Practice patterns and adverse events of nitrous oxide sedation and analgesia: a report from the Pediatric Sedation Research Consortium. J Pediatr. 2016;169:260-265.
12. Wilson S, Gosnell ES. Survey of American Academy of Pediatric Dentistry on nitrous oxide and sedation: 20 years later. Pediatr Dent. 2016;38(5):385-392.
13. Alzahrani AM, Wyne AH. Use of oral midazolam sedation in pediatric dentistry: a review. Pakistan Oral Dent J. 2012;32(3):444-455.
14. Azevedo ID, Ferreira MA, da Costa AP, et al. Efficacy and safety of midazolam for sedation in pediatric dentistry: a controlled clinical trial. J Dent Child (Chic). 2013;80(3):133-138.
15. Chopra R, Mittal M, Bansal K, Chaudhuri P. Buccal midazolam spray as an alternative to intranasal route for conscious sedation in pediatric dentistry. J Clin Pediatr Dent. 2013;38(2):171-173.
16. Lenahan M, Wells M, Scarbecz M. A retrospective study of 248 pediatric oral sedations utilizing the combination of meperidine and hydroxyzine for dental treatment. J Clin Pediatr Dent. 2015;39(5):481-487.
17. Kannikeswaran N, Mahajan PV, Sethuraman U, et al. Sedation medication received and adverse events related to sedation for brain MRI in children with and without developmental disabilities. Paediatr Anaesth. 2009;19(3):250-256.
18. Kip G, Turgut HC, Alkan M, et al. Clinical outcomes of different sedation techniques used in pediatric dentistry. Anaesth Pain Intens Care. 2016;20(1):13-16.
19. Coté CJ, Karl HW, Notterman DA, et al. Adverse sedation events in pediatrics: analysis of medications used for sedation. Pediatrics. 2000;106(4):633-644.
20. Nelson T, Nelson G. The role of sedation in contemporary pediatric dentistry. Dent Clin North Am. 2013;57(1):145-161.
21. Sabouri AS, Firoozabadi F, Carlin D, et al. Noise level measurement, a new method to evaluate effectiveness of sedation in pediatric dentistry. Acta Anaesthesiol Taiwan. 2014;52(4):169-175.
22. Lourenço-Matharu L, Ashley PF, Furness S. Sedation of children undergoing dental treatment. Cochrane Database Syst Rev. 2012;3. doi: 10.1002/14651858.CD003877.pub4.
23. Stringer KR, Bajenov S, Yentis SM. Training in airway management. Anaesthesia. 2002;57(10):967-983.
24. Sedation record. American Academy of Pediatric Dentistry. https://www.aapd.org/globalassets/media/policies_guidelines/r_sedationrecord.pdf Accessed January 3, 2019.
25. Daud YN, Carlson DW. Pediatric sedation. Pediatr Clin North Am. 2014;61(4):703-717.
26. America's health literacy: why we need accessible health information. U.S. Department of Health and Human Services. 2008. https://health.gov/communication/literacy/issuebrief/. Accessed December 28, 2018.
27. Kennedy PA Jr. Conscious sedation. J Pediatr.2002;
140(3):381-382.
28. Hills-Smith HL, Davis MJ. Conscious sedation in pediatric dentistry. N Y State Dent J. 1985;51(2):98-99.
29.Milnes AR, Maupomé G, Cannon J. Intravenous sedation in pediatric dentistry using midazolam, nalbuphine and droperidol. Pediatr Dent. 2000;22(2):113-119.
30.Dosani FZ, Flaitz CM, Whitmire HC Jr, et al. Postdischarge events occurring after pediatric sedation for dentistry. Pediatr Dent. 2014;36(5):411-416.
31. Council on Clinical Affairs. Protective stabilization for pediatric dental patients. American Academy of Pediatric Dentistry. http://www.aapd.org/media/Policies_Guidelines/BP_Protective.pdf. Accessed January 4, 2019.
32. White J, Wells M, Arheart KL, et al. A questionnaire of parental perceptions of conscious sedation in pediatric dentistry. Pediatr Dent. 2016;38(2):116-121.
33. Haas DA. Preparing dental office staff members for emergencies: developing a basic action plan. J Am Dent Assoc. 2010;141(suppl 1):8S-13S.
34. Pediatric anesthesia study. December 2016. Dental Board of California. https://www.dbc.ca.gov/formspubs/pedi_anesthesia_2016_r2.pdf. Accessed January 14, 2019.
35. Dental sedation regulations for your state or province. DOCS Education. https://www.docseducation.com/dental-sedation-regulations. Accessed January 4, 2019.